Pakistan posts 76 more coronavirus cases, no death
WHO countries seek better guard for next pandemic: Pfizer offers to sell medicines at cost to poorest countries
May 26, 2022 11:35 AM

Pakistan has registered another 76 coronavirus cases and no fatality during the last 24 hours (Wednesday), showed the statistics released by the National Institute of Health Pakistan on Thursday morning.
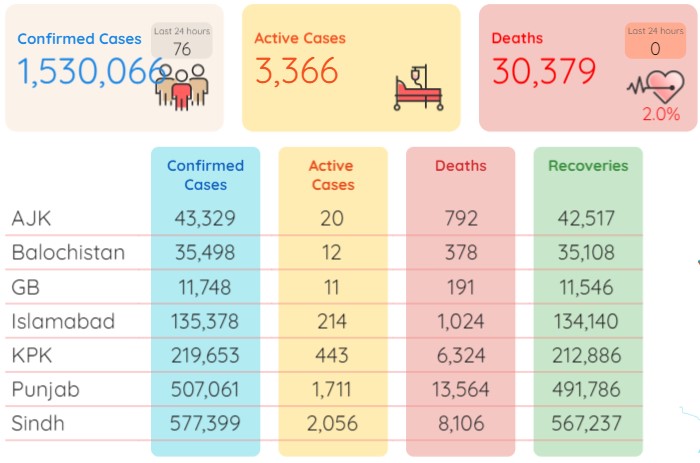
As per the latest NIH data, the death toll remained the same at 30,379, whereas the number of total infections now stood at 1,530,066 after adding the fresh 76 cases.
During the last 24 hours (Wednesday), 17,211 tests were conducted throughout Pakistan whereas the positivity ratio slipped to 0.44 percent. The number of patients in critical care was recorded at 75.
https://twitter.com/NIH_Pakistan/status/1529636516846239749
During the last 24 hours (Wednesday), another 98 people recovered from the Covid-19 and the number of total recoveries now stood at 1,496,321. As of Thursday, the total count of active cases in the country was recorded at 3,366.
As many as 577,399 coronavirus cases have so far been confirmed in Sindh, 507,061 in Punjab, 219,653 in Khyber Pakhtunkhwa, 135,378 in Islamabad, 35,498 in Balochistan, 43,329 in Azad Kashmir and 11,748 in Gilgit-Baltistan.
As many as 13,564 individuals have lost their lives to the pandemic in Punjab so far, 8,106 in Sindh, 6,324 in KP, 1,024 in Islamabad, 792 in Azad Kashmir, 378 in Balochistan and 191 in Gilgit Baltistan.
WHO countries seek better guard for next pandemic
Countries meeting at the World Health Organization this week are thrashing out how to prepare for future pandemics -- amid warnings that the planet is wide open to the next crisis.
WHO emergencies director Michael Ryan said Wednesday that infectious diseases were being amplified by weak public health services and poorly-managed urban settings.
Citing the monkeypox outbreaks in non-endemic locations, he told countries that the spread of the virus was "directly related to our inability, or unwillingness, to manage those risks earlier in their cycle of epidemic generation".
The Covid crisis laid bare major deficiencies in the global health system, and countries last year agreed numerous changes were needed to better prepare the world to face future threats.
At this week's annual World Health Assembly of 194 member states -- the WHO's decision-making body -- countries want some progress on filling the gaps in alertness and readiness that helped Covid spread worldwide, killing millions and trashing economies.
Ryan also warned about holes in surveillance.
Covid-19 testing has dropped off dramatically in many countries in recent months, meaning the virus could be spreading and mutating under the radar.
"We need data. We are becoming blind to the future of this pandemic and we are becoming blind to the emergence of others," Ryan said.
- World 'remains unprepared' -
WHO chief Tedros Adhanom Ghebreyesus warned countries that there was no time to lose.
"Building health emergency preparedness, response and resilience is an urgent priority because the pandemic has shown that the world was, and remains unprepared," he told the assembly.
Amendments are being considered to the International Health Regulations -- a set of legally-binding international laws governing how countries respond to acute public health risks.
And negotiations are under way towards a new "legal instrument" -- possibly a treaty -- aimed at streamlining the global approach to pandemic preparedness and response.
A progress report on the new instrument will be submitted at the 2023 World Health Assembly, with the final outcome presented for consideration at the 2024 WHA.
"A legally-binding instrument is a promise to future generations to ensure the world can respond to the next pandemic or health emergency," Tedros said.
The IHR, adopted in 2005, set out countries' rights and obligations in handling health emergencies that could spread abroad.
They also define what constitutes a so-called public health emergency of international concern (PHEIC) -- the highest alarm the WHO can sound.
- PHEIC shake flop -
The Covid PHEIC declaration on January 30, 2020 did little to shake countries into action and it was only when Tedros called the situation a pandemic on March 11 that many countries seemed to wake up to the danger.
The United States, the European Union, Britain, Japan, Australia and South Korea have brought forward a draft resolution on strengthening WHO preparedness for and response to health emergencies.
The US especially has insisted on the need to clarify roles and responsibilities, increase transparency and accountability, share best practices, and communicate in real-time on emerging problems.
The resolution would, among other things, seek to shorten dramatically the period between the adoption and implementation of IHR amendments, in a bid to speed up change.
"I am hopeful that we will reach consensus," said Loyce Pace, assistant secretary for global affairs at the US health ministry.
Countries and the WHO must do "everything that we can... to protect the global community from anything like this ever again", she told reporters.
The Covid pandemic "has been a nightmare that we've lived through, but if we don't do anything about it, then what are we here for?"
Pfizer offers to sell medicines at cost to poorest countries
US pharmaceutical giant Pfizer on Wednesday said it would sell its patented drugs on a not-for-profit basis to the world's poorest countries, as part of a new initiative announced at the World Economic Forum in Davos.
"The time is now to begin closing this gap" between people with access to the latest treatments and those going without, chief executive Albert Bourla told attendees at the exclusive Swiss mountain resort gathering.
"An Accord for a Healthier World" focuses on five areas: infectious diseases, cancer, inflammation, rare diseases and women's health -- where Pfizer currently holds 23 patents, including the likes of Comirnaty and Paxlovid, its Covid vaccine and oral treatment.
"This transformational commitment will increase access to Pfizer-patented medicines and vaccines available in the United States and the European Union to nearly 1.2 billion people," Angela Hwang, group president of the Pfizer Biopharmaceuticals Group, told AFP.
Five countries: Rwanda, Ghana, Malawi, Senegal and Uganda have committed to joining, with a further 40 countries -- 27 low-income and 18 lower-middle-income -- eligible to sign bilateral agreements to participate.
"Pfizer's commitment sets a new standard, which we hope to see emulated by others," Rwanda's President Paul Kagame said.
But he added that "additional investments and strengthening of Africa's health systems and pharmaceutical regulators" would also be needed.
- Seven years behind -
Developing countries experience 70 percent of the world's disease burden but receive only 15 percent of global health spending, leading to devastating outcomes.
Across sub-Saharan Africa, one child in 13 dies before their fifth birthday, compared to one in 199 in high-income countries.
Cancer-related mortality rates are also far higher in low and middle-income countries -- causing more fatalities in Africa every year than malaria.
All this is set to a backdrop of limited access to the latest drugs.
Essential medicines and vaccines typically take four to seven years longer to reach the poorest countries, and supply chain issues and poorly resourced health systems make it difficult for patients to receive them once approved.
"The Covid-19 pandemic further highlighted the complexities of access to quality healthcare and the resulting inequities," said Hwang.
"We know there are a number of hurdles that countries have to overcome to gain access to our medicines. That is why we have initially selected five pilot countries to identify and come up with operational solutions and then share those learnings with the remaining countries."
- 'Very good model' -
Specifically, the focus will be on overcoming regulatory and procurement challenges in the countries, while ensuring adequate levels of supply from Pfizer's side.
The "not-for-profit" price tag takes into account the cost to manufacture and transport of each product to an agreed upon port of entry, with Pfizer charging only manufacturing and minimum distribution costs.
If a country already has access to a product at a lower price tier, for example vaccines supplied by GAVI, a public-private global partnership, that lower price will be maintained.
Hwang acknowledged that even an at-cost approach could be challenging for the most cash-strapped countries, and "this is why we have reached out to financial institutions to brief them on the Accord and ask them to help support country level financing."
Pfizer will also reach out to other stakeholders -- including governments, multilateral organizations, NGOs and even other pharmaceuticals -- to ask them to join the Accord.
It is also using funding from the Bill & Melinda Gates Foundation to advance work on a vaccine against Group B Streptococcus (GBS), the leading cause of stillbirth and newborn mortality in low-income countries.
"This type of accord is a very good model, it's going to help get medicines out," Gates told the Davos conference, adding that "partnerships with companies like Pfizer have been key to the progress we have made" on efforts like vaccines.
With inputs from AFP.




 Yet another burden on people: Govt hikes oil prices
Yet another burden on people: Govt hikes oil prices Foreigners safe after suicide-bomber targets their van in Karachi
Foreigners safe after suicide-bomber targets their van in Karachi Public reacts to Bohemia's music video ‘Salsa’ starring Sistrology
Public reacts to Bohemia's music video ‘Salsa’ starring Sistrology Saudis offered PIA, airports, joint ventures to build five-star hotels
Saudis offered PIA, airports, joint ventures to build five-star hotels Finance minister rules out further rupee devaluation
Finance minister rules out further rupee devaluation Mehar Bano and Mamya Shajaffar’s bold dance videos invite public's wrath
Mehar Bano and Mamya Shajaffar’s bold dance videos invite public's wrath




